Understanding Katie....
Regular
readers of this blog will know how long it took us to get a diagnosis
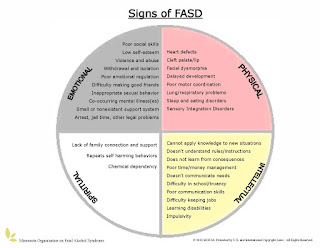
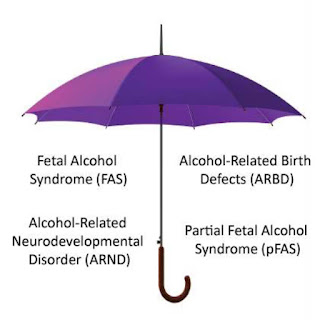
of Alcohol Related Neurodevelopmental Disorder (ARND), which is a
diagnosis under the Foetal Alcohol Spectrum Disorder (FASD) umbrella,
and ADHD. It took us a while to realise that her challenges and
behaviour weren't age related and "just" adoption related.
There is, of course, never a "just" when it comes to
adoption but it can be easy to miss other diagnoses when you're
seeing through adoption spectacles because they can tend to blur
other issues. Let's face it, it's hard enough to wrap your adopter
head around trauma and attachment issues let alone then working out
what else might be going on for our children. Most adopters I
know spend a lot of time watching their children and worrying that
they might be missing something. You tie yourself up in knots
trying to work out why your child is doing this or that and whether
you should be doing something about it but then not quite sure who to
ask and where to access support.
It's
a real minefield when it comes to FASD with very few doctors trained
in diagnosing the condition. A diagnosis of FAS (Foetal Alcohol
Syndrome) is possible via a genetics referral but only if the child
has all the facial features associated with the full blown syndrome.
Only a small percentage of children have the full blown syndrome and
symptoms can vary depending on when during the pregnancy the baby was
exposed to alcohol. As a parent in the UK you are lucky if you
can find a GP who has actually heard of FASD let alone then be able
to access a referral onto someone who is able to diagnose the
condition.
We
were lucky - well lucky and very tenacious. Our GP had never
heard of FASD, in fact he wrote ASD in his notes - I had to stop him
and inform him that we weren't talking about Autistic Spectrum
Disorder. We managed to find a paediatrician locally who was trained
in diagnosing FASD through our own resources and agreed to take our
our referral. I then went back to the GP with the details in my
sticky fingers and asked him to make the referral. Being used
to my dymanic approach, he agreed.
Having
accessed a paediatric referral and received a diagnosis of ARND and
ADHD we have turned our attention to trying to understand exactly
what this diagnosis means to Katie's functioning. We can easily
see her distractability. We know the full force of her
behavioural challenges. We watch her struggle with OCD and
panic attacks due to anxiety. We are starting to understand that she
has processing difficulties but what is driving those co-morbidities?
Fed up with her teachers at school telling me "she's fine at
school" but seeing the stress that she experiences through a
general school day I decided to start finding this out for myself.
I
spend a fair bit of time these days reading up about FASD and asking
what other people are doing to help their children with this
diagnosis. There are so many symptoms and co-morbidities that it can be hard to know. What other information do we need? It really
is a case of piecing it all together because my GP doesn't have a
clue. Other than a small head circumference we have ascertained
from our paediatrician that Katie has no other physical difficulties
except for mild hypermobility. From talking to other parents I
learned that with FASD it's often common to have sensory processing
challenges as well so that was where I instinctively turned my attention
next. I contacted our Post Adoption Social Worker (PASW) to ask
if we could access an assessment from an Occupational Therapist via
the Adoption Social Fund (ASF) and I also made an appointment
independently with a Behavioural Optometrist. Initially the ASF said
they would not fund the OT assessment if the issue was related to a
physical difficulty but they would fund it if it the assessment was
due to trauma. I noted back to our PASW that if being fed
alcohol in the womb against your will and receiving a diagnosis of
ARND as a result wasn't a trauma then I didn't know what else could
be. Thankfully this viewpoint was upheld by the ASF and funding was
secured for a full OT assessment towards the end of the school
holidays.
Whilst
we were waiting for the OT assessment I took Katie to meet with a
Behavioural Optometrist. This was something I had been recommended to
do by a friend who's son has a diagnosis of ADHD and it had been
found to be very helpful. This assessment has to be self funded
because, despite it being enormously helpful and quite possibly one
of the most helpful services we have accessed, we have been told it
is not funded by the ASF which is highly frustrating because the cost
of this service in our local area is quite high. To deny Katie a
service that might actually help her makes me feel very puzzled.
 The
assessment was enlightening in itself and highlighted that Katie's
brain processes in relation to her vision are compromised due to the
brain damage and her delayed brain development in some areas. Whilst
she can see perfectly well her visual processing takes in too much
information and struggles to maintain focus and is easily distracted.
The easiest way of describing it is to say she sees everything
and nothing. Her brain is on permanent sensory overload which
impacts heavily on her executive functioning. If you ask her to find
a pair of shoes in a cupboard or tidy her room she is unable to
pinpoint where those shoes are because she can't see the wood for the
trees. She also pre-empts a lot what might be coming next, her
brain jumping about in anticipation. I also saw first hand how
easily she becomes anxious when her perception of a situation is
challenged and how this then impairs her ability to think clearly and
function well. Watching the Behavioural Optometrist assessing
her was fascinating. We had chosen to go for a 45 minute assessment
rather than the several hours long one because I didn't feel Katie
would be able to cope and I was correct in that judgement. She was
incredibly cooperative (as she always is with other people) but was
clearly very strained by the end of the assessment and unable to hold
her hyperactivity together.
The
assessment was enlightening in itself and highlighted that Katie's
brain processes in relation to her vision are compromised due to the
brain damage and her delayed brain development in some areas. Whilst
she can see perfectly well her visual processing takes in too much
information and struggles to maintain focus and is easily distracted.
The easiest way of describing it is to say she sees everything
and nothing. Her brain is on permanent sensory overload which
impacts heavily on her executive functioning. If you ask her to find
a pair of shoes in a cupboard or tidy her room she is unable to
pinpoint where those shoes are because she can't see the wood for the
trees. She also pre-empts a lot what might be coming next, her
brain jumping about in anticipation. I also saw first hand how
easily she becomes anxious when her perception of a situation is
challenged and how this then impairs her ability to think clearly and
function well. Watching the Behavioural Optometrist assessing
her was fascinating. We had chosen to go for a 45 minute assessment
rather than the several hours long one because I didn't feel Katie
would be able to cope and I was correct in that judgement. She was
incredibly cooperative (as she always is with other people) but was
clearly very strained by the end of the assessment and unable to hold
her hyperactivity together.
The
Behavioural Optometrist immediately reported back that he could see
how quickly she questioned her knowledge and how her anxiety
prevented her from being able to access information from her brain.
This was noted when he asked her to cover her left eye with a
lens. Katie covered her right eye so he asked her which eye
she was covering. She replied her left and he then asked her to
tell him how she came to that information. I was confused at
this point because usually she knows her left and right fairly
reliably. You could see she was confused and I attempted to jump in
to help her but the Optometrist asked me to hold off. He then
asked her if she was left handed. She looked confused and then
said that she was. He then asked her if she had always been
left handed and she said "yes" but looking very confused at this
point. He asked her how she knew which was her left and right.
She put both hands up to make an L shape but still got
confused. He pointed out to me after the assessment that, due to her
anxiety about the task, she was unable to access the knowledge she
had about which was left and right so ended up questioning everything
she knew about this.
 We
have seen this before when a friend at school told Katie she didn't
have a cat. She was very upset about this because she does have
a cat (we now have 4). At home I asked her if she had a cat and
she said she did but because her friend questioned this fact and told
her that she didn't she got so confused she was unable to argue her
point or even know what the truth was. Imagine an older child
or young person with FASD being queried about an event or something
about them by the police and giving an inconsistent statement because
they literally cannot access the truth from their brain due to
anxiety and brain damage. It made me realise just how vulnerable my
daughter might be in the future without the right help now.
We
have seen this before when a friend at school told Katie she didn't
have a cat. She was very upset about this because she does have
a cat (we now have 4). At home I asked her if she had a cat and
she said she did but because her friend questioned this fact and told
her that she didn't she got so confused she was unable to argue her
point or even know what the truth was. Imagine an older child
or young person with FASD being queried about an event or something
about them by the police and giving an inconsistent statement because
they literally cannot access the truth from their brain due to
anxiety and brain damage. It made me realise just how vulnerable my
daughter might be in the future without the right help now.
The
findings of the Behavioural Optometrist were backed up by the OT when
she assessed Katie. Thankfully all Katie's sensory development is age
appropriate which ticks one problem off the tick sheet. The
conclusion of the OT was that Katie is very inattentive so gave her a
diagnosis of ADD, without the hyperactivity element. It isn't
commonplace these days to diagnose using that terminology. ADHD is
an umbrella diagnosis rather like FASD but her description was
helpful nonetheless. Knowing that her hyperactivity and distraction
is driven by external stimuli rather than internal helps us find a
plan to support her. The OT recommended that Katie access a
prescription for atomoxetine (also known in the UK as Strattera)
which she feels will dampen down the external onslaught and hopefully
give Katie's brain the space it needs to develop. Currently the
sensory overload is preventing her accessing her memory effectively
and is causing her to be highly anxious. I'm curious as to how that
will impact (or not) on any brain damage caused by the alcohol
exposure but I suspect that will become clear over time.
 So
how do we accessing atomoxetine? Back to the drawing board, although
it was a drawing board slightly confused by the OT who didn't think
our Paediatrician would be able to prescribe atomoxetine and
recommended we access CAMHS (I do love a pipe dream!). To cut a very
long few weeks and a self referral to CAMHS short I have now
ascertained that our Paediatrician can prescribe said drug so an
appointment is pending. I'm going to leave our referral to CAMHS
ongoing because there is still the issue of a recommended full
psychological evaluation to sort out and to examine her executive functioning and I think we need a referral
to CAMHS because Katie's anxiety is impacting on her eating, sleeping; behaviour and mood. This post is already long enough so I won't go into great
details about that but parents with a child under the FASD umbrella
will know how intense and stressful it is parenting a child with this
condition. Let's just say there isn't much rule following going on
here at the moment along with lots of oppositional behaviour.
Thankfully the temper tantrums have calmed down considerably although
have recently been replaced by panic attacks where she is convinced
she is going to be sick. Being sick is one of Katie's biggest fears
along with food being out of date and her new one of the house being
broken into (thank you to the would be burglars who broke into Nana's
house for that new fear – thankfully her house is empty pending the
sale so nothing was stolen and no-one hurt).
So
how do we accessing atomoxetine? Back to the drawing board, although
it was a drawing board slightly confused by the OT who didn't think
our Paediatrician would be able to prescribe atomoxetine and
recommended we access CAMHS (I do love a pipe dream!). To cut a very
long few weeks and a self referral to CAMHS short I have now
ascertained that our Paediatrician can prescribe said drug so an
appointment is pending. I'm going to leave our referral to CAMHS
ongoing because there is still the issue of a recommended full
psychological evaluation to sort out and to examine her executive functioning and I think we need a referral
to CAMHS because Katie's anxiety is impacting on her eating, sleeping; behaviour and mood. This post is already long enough so I won't go into great
details about that but parents with a child under the FASD umbrella
will know how intense and stressful it is parenting a child with this
condition. Let's just say there isn't much rule following going on
here at the moment along with lots of oppositional behaviour.
Thankfully the temper tantrums have calmed down considerably although
have recently been replaced by panic attacks where she is convinced
she is going to be sick. Being sick is one of Katie's biggest fears
along with food being out of date and her new one of the house being
broken into (thank you to the would be burglars who broke into Nana's
house for that new fear – thankfully her house is empty pending the
sale so nothing was stolen and no-one hurt).
Katie's
OT came into school last week to do a class observation and
perception test. It only took her 20 minutes in class to see Katie
misunderstand instructions. The class had been asked to copy down
the days of the week in French, randomly written on the whiteboard
and list them in the correct order in their workbooks. All Katie
heard of the instruction was to copy the words down, and that is what
she did, as a mirror copy of the way they were written on the board.
When I asked Katie about the task later on that day she was genuinely
convinced she had completed the task correctly. This explains why
she doesn't often ask for help - she doesn't realise she's misunderstood. The way we have agreed to help her
with this in school is for the teacher to provide a sheet on the
table for small group work with the task written on it so Katie can
re-read it. This also ensures she doesn't feel singled out. School
have agreed to use small groups where possible instead of whole class
teaching and approved the use of fiddle toys. We are going to pin
fiddle things such as material or soft keyrings into her pockets to
keep them discreet. The use of LSA support was noted. Because there
is a lot of pressure on the class LSA due to the needs of another
pupil this will need to be assessed by the school. Katie doesn't
meet the level of need required for an EHCP plan because she doesn't
need one-to-one support so this, I suspect, will be a challenge for
school. I'm hoping that once the other pupil gets the diagnosis
needed to meet the need for an EHCP that additional funding might
come out of that and free up the current LSA. I'll have to stay on
top of that though.
So
that's where we are currently: Pending an appointment with the
Paediatrician; waiting with fingers tightly crossed that we will meet
the criteria for our local CAMHS service; watching to see how school
work with the recommendations of the OT; and deciding what we can do
about working with the Behavioural Optometrist.
 One
positive that we experienced this week was that we realised there was
a link between Katie feeling sick and panicky on a Monday before
going to Brownies. Because the Brownie pack has moved to a new hall Katie is
struggling with the transition; the new smells; the new hall and this
is raising her anxiety levels. After helping her through screaming
and hysteria where she wouldn't believe she wasn't going to be sick
this has been a massive realisation and enabled her to go to Brownies
with a little Cherry Plum Bach Flower Remedy to help calm her down.
She is beginning to understand that anxiety for her feels like she's
going to be sick. We have a way to go with this but I'm pleased she
finally is able to hear what I'm saying to her and know that we can
help her through it.
One
positive that we experienced this week was that we realised there was
a link between Katie feeling sick and panicky on a Monday before
going to Brownies. Because the Brownie pack has moved to a new hall Katie is
struggling with the transition; the new smells; the new hall and this
is raising her anxiety levels. After helping her through screaming
and hysteria where she wouldn't believe she wasn't going to be sick
this has been a massive realisation and enabled her to go to Brownies
with a little Cherry Plum Bach Flower Remedy to help calm her down.
She is beginning to understand that anxiety for her feels like she's
going to be sick. We have a way to go with this but I'm pleased she
finally is able to hear what I'm saying to her and know that we can
help her through it.Useful Links for FASD:
FASD Trust
NOFAS UK
FASD Network
FASD Clinic
Adoption UK - Living with FASD
British Association of Behavioural Optometrists
FASD Through My Eyes



thanks for such a comprehensive journal into your life with your daughter - fascinating and helpful reading - thanks so much!
ReplyDeleteThank you for this post. This has given me food for thought as far as Missy is concerned.
ReplyDeleteThis is a great post - parenting a child with FASD requires us to be detective, researcher, advocate all while parenting a child with complex needs. You are doing an amazing job - all good wishes to you. Never heard of a 'behavioral optometrist' before - will definitely look into that.
ReplyDeleteI don't have anything useful to say but just want you to now that I read your pots and I'm rooting for Katie and for you. xxx
ReplyDeleteTotally understand. We have a daughter with almost identical issues. We just want her future, like you do for Katie, to be ss 'normal' as possible. Let's pray it's not a pipe dream and keep working for that. Thank you for your honesty and tenacity.
ReplyDeletereally interesting - thank you for this. Our grandson who has fasd struggles to put words together to make sentences to express himself, and again we think that the stimuli coming from speech is overwhelming - he can pick out what he needs to do, but you notice odd things like he doesn't know about back and front when it isn't related to HIS back and front. So front curtains are any curtains facing his front, not at the front of the house. It's like putting one of those refracting specs on to contemplate how he's interpreting speech.......! Well done for all the wondering and detective work: our children are very different but looking at how they function can help us understand the difficulties more fully - lots of food for thought. Good luck Kaiet: hope that Brownies is ok now.x
ReplyDeleteMy child has ASD and lots of processing problems/difficulties remembering simple instructions (although appears very clever). Also high anxiety round unfamiliar transitions. You are doing brilliantly to find all this out, just knowing it will make a big difference to your ability to help Katie. Especially when you feel like screaming, YOUR SHOES, you need to PUT YOUR SHOES ON! [sorry a familiar scene of hall rage in our house, which we are trying to put an end to, and it IS GETTING BETTER]
ReplyDeleteBoth my sons would do the task as you describe Katie doing. It is not because they are not following instructions, but because they follow the literal instruction rather than the implicit instruction. Correct order literally means to them the order they are written in. 16 year old with dyspraxia has just answered a Business Studies A level question on pricing strategy by writing about the cost of marketing and advertising. Price to him literally meant money. He is otherwise intelligent. But issues like this can cause so much stress unless it is broken down by the teacher, and you talk through [social stories?] some of the ways people can mean one thing or tease or joke without it literally being true. Ditto the cat story. It is a form of banter children often use that gets completely misunderstood by our children. Even professionals will ask questions that children want to answer "correctly" and they give the answer they think they are meant to give and the [stupid] professionals don't even realise this when they ask the question. I personally am completely confused by people like driving instructors ask me whether I intended to turn left or right in a semi confrontational testing way = I get flustered and incredibly anxious. My children hate being assessed - it brings out the absolute worst in them.
ReplyDeleteYou can apply for an EHCP without the school supporting you. I would suggest you do straightaway, whatever they say; it might actually increase the support they offer. Do NOT be fobbed off by them saying that her level of need is not great enough = school is making her extremely anxious, that is a high level of need. She is well behaved because she is frightened of getting something wrong, and as you say, she is indeed getting "things wrong" both socially and academically, because she is not supported enough, because they do not have the funds, because they do not have an EHCP for her.